Welcome to DSAP.net
DSAP - Disseminated Superficial Actinic Porokeratoses (porokeratosis)
3/24/2020 NEW: Topical cholesterol/lovastatin treatment (Scroll down to the blue box)
4/23/2022 NEW: 2019 study regarding chemical peels (Scroll down to "Chemical peel")
10/22/2023: Better explanation on how to use masking technique with sunless tanner, concealer, tissue.
4/7/2024: More clarity on freezing. I think it makes sense for those with light skin and permanently red spots.
DSAP is an uncommon genetic skin disorder that seems to get misdiagnosed much more often than not. I am not a doctor, but I've learned from experience that amazingly (and sadly) the majority of Dermatologists haven't even heard of DSAP or just plain can't recognize DSAP. General practice doctors? Forget about it! I found this out the hard way, learning 6 years later that I had some of these genetically predisposed spots that are generally brought on by sun exposure.
Amazingly I had visited one family physician and four dermatologists over the years before I finally got the correct diagnosis. These various doctors misdiagnosed it as a fungus, "nothing", seborrheic keratosis, folliculitis, actinic keratosis (AKA solar keratosis). One dermatologist did a biopsy for cancer before concluding that my skin condition was "nothing". More recently, a 5th dermatologist of over 20 years, whom I told up front that I had DSAP, nevertheless amazingly misdiagnosed me as having "skin inflammation caused by overexposure to an irritating chemical or physical agent" (AKA "irritant contact dermatitis") and prescribed topical steroids and petroleum jelly! So 5 out of 6 dermatologists each diagnosed me as having 5 other conditions! That doesn't count a 7th dematologist who had never heard of DSAP when I inquired by phone. What does that say about the competence of medical professionals?
With so much misdiagnosis, this also suggests that DSAP is less 'rare' than advertised. Dermatologists most commonly misdiagnose DSAP patients as having AK (actinic keratosis), which is a much more serious condition. I beleive there must be more than a few DSAP patients out there who, because of misdiagnosis, mistakenly believe that they have actinic keratosis.
I have received emails from people who have been misdiagnosed as having psoriasis, SCLE and even lupus of the skin.
SUSPECT GENES HAVE BEEN IDENTIFED, BUT FURTHER GENETIC RESEARCH IS NEEDED TO CONFIRM THE CAUSATIVE GENE IN MORE PATIENTS WITH DSAP AND UNCOVER THE FUNCTIONAL MECHANISMS
Any actual cure for DSAP will have to correct the underlying genetic error(s) via stem cell therapy or gene editing. These revolutionary technologies are in their infacy, but growing rapidly. Any gene therapy begins by identifying a well-defined disease gene. Fortunately, there have already been two important genetic studies, both coming out of China.
In 2000, a study of a family effected by DSAP found a locus (location on a chromosome) for a DSAP gene. This 2000 study was apparently valuable in helping with a 2012 Chinese study which identified a gene (mevalonate kinase gene) responsible for DSAP in 2 people from the same family. According to this site, mutations in the mevalonate kinase (MVK) gene, located to chromosome 12q24, have been found in up to one-third of DSAP cases. I assume that this one-third figure was based on subjects from one or both of the Chinese studies. Detailed PDF document
MVK gene mutations identified by the 2012 study offer the best candidate targets for clinical treatment of the disease (such as gene therapy).
Scientists from this 2012 study say that DSAP exhibits high genetic heterogeneity [Heterogeneity means different gene mutations (changes) cause the same disease or condition]. But, does that mean that multiple genes may be at play for any one particular patient, or that only one of several genes may be the culprit for any one particular patient? The 2012 study speaks of exome sequencing being effective at identifying monogenetic diseases. Monogenic disorders are caused by variation in a single gene (Examples of monogenetic disorders include sickle cell anemia, cystic fibrosis, Huntington disease, and Duchenne muscular dystrophy). The 2012 study actually speaks of five 'linkage loci' for DSAP [Loci are locations of genes on chromosomes]. Presumably, more genetic studies are needed to confirm these as causative genes.
12q23.2–24.1
12q24.1–q24.2
15q25.1–26.1
1p31.3–p31.14
16q24.1–24.35
I am not sure if it was one single gene defect for each patient, or if some patients studied had more than one of these linkage loci.
The SLC17A9 gene (on chromosome 20q13.33) was found to have a disease causing role in two families with DSAP. I have not found any information on what percentage of patients have this particular gene defect.
The 2012 study concluded that "Further studies are needed to confirm the causative gene in more patients with DSAP and uncover the functional mechanisms". Because genes can have multiple roles, turning genes on and off can have major unintended consequences. That is why it is important to figure out the functions of a gene.
"We demonstrate a pathogenic role for SLC17A9 in two DSAP families. The probable mechanism may be associated with abnormal ion influx/efflux of transmembrane Ca2+ and accompanying ATP release. Further studies are needed to confirm the causative gene in more patients with DSAP and uncover the functional
mechanisms."
To sum it up, genes can have many roles and functions. Turning genes on and off can have huge, unintended consequences. That is why further genetic studies (with larger pools of DSAP patients) are needed.
Gene therapy holds the best hope
Hopefully, there will be a gene therapy for DSAP one day. There are gene therapies for other disorders going on right now! It can take many years (even decades) for a gene therapy to move from discovery, to preclinical trials, clinical trials, and then to approval for public use.
As of February 2021, there were 10 approved gene therapies. As of February 2023, there were 27 approved gene therapies in the US. Gene therapy applications are expected to double each year. More than a thousand stem cell and gene therapies were in development as of Jan 2022. More than a thousand product candidates are being evaluated in clinical trials worldwide. The global cell and gene therapy market size was around US$18.6 billion in 2022 and is projected to hit around $94 billion by 2030.
In 2007 the cost of a human genome sequence is about one million dollars. As of December 2022 it was down to only about $600. This makes genetic studies much more attainable.
One thing that might hamper progress on gene therapy is the mere fact that DSAP is an uncommon condition. How uncommon, I am not sure. Because misdiagnosis is so common, DSAP may be more common than uncommon. Obviously, the more people affected by a disorder, the more financial incentive to develop a treatment. Although, for whatever reason, there are indeed some companies whose focus is on rare diseases. China has been seemingly undeterred by their research efforts.
Another problem is that cell and gene therapies are currently very expensive. Analysis by the Institute for Clinical and Economic Review (ICER) suggests the average cost of a gene therapy is between $1 million and $2 million per dose. This site says that the cost can range from $400,000 to $2 million. However, cutting edge technology is always expensive in the beginning. One has to believe that the cost will come way down in years to come.
Also, when you hear stories about gene therapies for rare skin conditions like this one, this gives us hope.
Monoclonal antibodies may have potential therapeutic applications in the treatment of autoimmune diseases.
Can you help?
If anyone reading this is an expert in genetics, perhaps you can help answer some questions, as I am trying to better interpret the Chinese studies.
WANTED: Research scientists
In order to get funding from organizations, government, philanthropist donors, and/or corporate donors, you generally need to already have people in place who want to work on the project. Accordingly, I am trying to round up indications of interest from such researchers, doctors, experts in genetics, University professors and anyone else who can help.
Do you have friends or family who are knowledgeable in the field of genetics? Knowledge in working with contract research organizations? If you speak Chinese, it would help to learn more about what is happening in China with regard to research.
Either way, please join my mailing list so that I can notify you of new DSAP related developments (major new studies, treatments, gene identification studies, etc). If you were participate in a gene study it would certainly be beneficial to learn what specific gene(s) is causing your DSAP.
TREATMENTS
For now, doing your best to keep out of the sun, and wearing the highest SPF sunscreen (if you must be out in the sun) is the best 'treatment'. Remember that sunscreen only works to an extent -- Short walks that you must take are OK. Long walks are illadvised.
I can personally report that these good sun avoidance habits help a lot! From my experience, hyper pigmentation is greatly reduced, and the thickness of threatlike-borders gets improves. There is significant improvement, especially if you had until only recently been getting lots of everyday sun exposure. This improvement plays out over months and years, so don't lose hope.
I should also mention that you want to avoid irritating DSAP spots. Don't pick at them. Don't get scraped up while doing gardening work. This may cause spots to become permanently hyperpigmented or take many months for the redness to subside.
Further down the page, I talk about the various off-label medications and treatments that have been used to improve the appearance of DSAP. Aside from cholesterol/lovastatin, and Dovonex (uncommon), are these meds worth it? I don't think so. The big elephant in the room is that the genetic error still remains. Think of mowing a lawn that keeps growing back. I think that at best, you are merely temporarily suppressing genetic expression. Nevertheless, untill a gene therapy emerges, it would be nice if a suppressive medication that works better than cholesterol/lovastatin was created specifically to target DSAP.
Medications/action possibly worth trying?
As previously mentioned, the 2012 study found that DSAP exhibits a high degree of heterogeneity. This probably explains why some meds may help some patients, while doing nothing for others.
1. Topical cholesterol/lovastatin or just lovastatin 2%. In my opinion, this is the best, and for some, maybe only medication that actually significantly improves DSAP if used on an ongoing basis. It works very well on milder DSAP spots -- not on entrenched lesions or red, irritated spots. 1) It's a prescription topical gel mixed at an apothecary (AKA 'compounding pharmacy'), 2) It's not a 'brute force' type medication, in that there should be no harsh skin reaction, and 3) It's very low cost. After just 3 to 4 weeks of treatment, this medication produced noticeable improvement on my arms, in that it significantly reduced the threadlike borders of DSAP spots. However, once I stopped using this medication, the improvement only lasted about a month. Accordingly, this medication must be used on an ongoing basis about once per day to maintain improvement. Beware of medical journal headlines that boast of "Successful Treatment" using cholesterol/lovastatin, suggesting that a one-time regimen leaves you cleared up for good.
For most patients, there is a very noticeable improvement. For me, the threadlike borders on some spots on my arms have completely disappeared, and the overall rough texture of DSAP is much improved. However, this med does not do very much to improve the problem of clogged pores.
One person reported to me that this medication did nothing. Another reported that their spots became more inflamed/red/irritated. As previously mentioned, this med is generally for milder DSAP spots. From my experience, this medication is not well tolerated on spots that are already red and irritated, and it does nothing to improve slightly hyper-pigmented spots. Also, it may have a very limited effect on spots on your legs. I choose not even to bother to continue using it on my legs.
One concern is that this medication could cause fattening of the liver if you apply a lot. For this reason, I would only use it sparingly on small areas that bother you the most -- perhaps select spots or areas on your arms. Ask your doctor if you want to use this medication on an ongoing basis. My doctor says that in small doses, fattening of the liver should not be a concern. It took me 2 1/2 years to use up a 60-gram jar! I've discovered that you do NOT need to apply liberal amounts of this medication for it to do its thing. If after rubbing it in, you still see residual moisture that is not being absorbed, you are using too much. Also, keep in mind that a portion of topical medications will simply be exfoliated as dead skin -- not all eventually processed by the liver.
For more details on cholesterol/lovastatin see the blue box below.
2. Apparently in very uncommon cases, Tacalcitol may work for DSAP. As far as I know, it is not a brute force-type medication that causes a harsh reaction such as redness. Reports are sketchy. See "Dovonex / Tacalcitol / Calcipotriol" below. For that reason, I believe it's at least worth a try. Start with just a couple of test spots or a small test area. There is no point in using this drug over large areas to start, because odds are that it just won't do anything. If it does happen to work for you, the next question is how long does the improvement actually last for? Since I have not heard from one single patient who had success with this medication, I just don't know. My hunch is that when it works, it's no different than cholesterol/lovastatin -- Stop using it and within a month you're back to square one again.
3. You might or might not consider freezing or laser treatment of the most troublesome, entrenched and/or red spots. I've received mixed feedback from patients. Some of the negative reports regarding freezing seem to be due to the doctor not freezing deep enough. For those with lighter skin, I believe that freezing makes great sense for treating spots that have turned permanently red without improvement. If you do try freezing or laser treatment, then save yourself the aggravation by only doing so at the onset of Winter, when the red scars will be covered up and you will have several months to heal up.
3/24/2020 New suppressive DSAP medication: Topical cholesterol/lovastatin
Low cost, not a harsh treatment, good improvement (for most), but will revert back to prior state if you discontinue using this medication
 Click here for details. Click here for PDF file details on the study. I was initially pleased with topical cholesterol/lovastatin. For starters, this report comes from the highly reputable Yale University School of Medicine. 3 out of 4 patients who I had communicated with by email, had very positive things to say about this medication mixture. And this medication is relatively cheap -- as low as $59 for 226 grams (or 8 ounces). The recommendation is to use cholesterol/lovastin morning and night for 2 months, but for up to 3 months as may be needed. From my experience, you can use it as little as once per day for about 3 or 4 weeks to reach maximum benefit. If you want to maintain the improvement, I estimate that you only have to use it between once a day to once every 2 days.
Click here for details. Click here for PDF file details on the study. I was initially pleased with topical cholesterol/lovastatin. For starters, this report comes from the highly reputable Yale University School of Medicine. 3 out of 4 patients who I had communicated with by email, had very positive things to say about this medication mixture. And this medication is relatively cheap -- as low as $59 for 226 grams (or 8 ounces). The recommendation is to use cholesterol/lovastin morning and night for 2 months, but for up to 3 months as may be needed. From my experience, you can use it as little as once per day for about 3 or 4 weeks to reach maximum benefit. If you want to maintain the improvement, I estimate that you only have to use it between once a day to once every 2 days.
Mostly positive feedback from patients who visit this site
One person reports using topical cholesterol/lovastatin for the last 10 weeks. They report that their skin is much, much smoother. Characteristic ridges are gone and less redness, especially on the newer spots. They also know of two other DSAP patients who have experienced very good results. This patient reports that those spots that became redder from using the cream are also the ones that diminished faster.
Another patient reports that nothing has ever worked as well as this medication. They have been using it for the last 2 1/2 months. DSAP spots that had been there for decades have faded. Their doctor suggested morning and night application, however this patient says that this was too often and caused itching. Once per day worked best. After 2 months they reduced to once every other day. This patient reports some redness and irritation when they first started treatment. After 5 days of applying it twice a day to both legs, they reduced to once a day on one leg only. Things then "settled down". This patient says that "more is not better". After 2 months they reduced to every other day.
A third patient reports the thread-like borders of DSAP being gone after just one week of application, and that their arms and legs felt very smooth. They report that the spots are still there but have faded.
However, a fourth patient developed a harsh reaction of itching, increased redness, stinging / burning when applied to legs. Note: I do not recommend using any medication that causes a harsh reaction. This medication is probably not recommended for DSAP spots that are red and irritated.
Another patient reported very minimal benefit or no benefit after 8 weeks of treatment.
Improvement for me too, but short-lived once stopped
I used this topical treatment on a few test spots and areas for 10 weeks. For me, it worked very well on spots on my forearms, which for the most part, have little to no hyperpigmentation (redness). These spots began showing improvement after just 1 to 2 weeks. I probably could have stopped using this medication on my forearms after just 3 or 4 weeks! Yes, the DSAP spots were still there but the threadlike borders faded very noticeably. Skin was also just generally much smoother. I'm not sure if there was any additional improvement to forearms in weeks 5 through 10 of treatment.
I should note that hardened / raised pores (that may be effected by DSAP) do not seem to respond well (or at all) to this medication.
Spots on my legs seem to be least responsive to this treatment. There was some improvement, but not worth continuing.
Unfortunately, once I stopped applying the medication, the improvement only lasted for about a month. The thread-like borders returned. Now, I only use it for select spots/areas of my forearms.
Side effects?
People react differently to medication.
One patient relays to me that a pharmacist said that sometimes there is redness at first, but then it should subside. When I started using topical cholesterol/lovastin on test areas, within about a day of use, it caused a couple of spots that were already red to become redder and irritated. Out of an abundance of caution I completely stopped applying to just those spots. After 5 days of use, some spots with no hyperpigmentation started to show some redness. And so I briefly reduced to once per day, then back to twice per day. For me, the redness never returned. I believe that if you have spots that are already red, then this medication is not right for you. For DSAP with hyperpigmentation, your best course of action is to focus on minimizing sun exposure and wearing SPF100 sunscreen if you are out and about.
One patient reported itching when using twice per day and so they reduced to once per day. I have not experienced any itching from using this topical med.
If you experience minor issues such as itching, redness or other irritation then you can reduce to once per day, then try going back to twice per day. If you experience a very harsh reaction, then I would discontinue use. My doctor says to do what works for you.
Another concern, whether founded or not, is that one patient has reported to me that their dermatologist had questions whether this treatment could cause a fattening of the liver as a side effect. I have not heard back from this patient regarding these concerns. I am not a doctor, but from my Internet research, statins can cause liver damage. However the information I have found is in regards to patients taking Lovastatin in oral pill form. For DSAP, you would be using it topically and so perhaps some of the drug is eventually excreted by exfoliation of skin. The body can and does absorb through the skin, then eventually the liver would be largely responsible for metabolizing lovastatin. More importantly, when taken as a pill, patients usually take upwards of 20 to 80 mg of lovastatin per day. With cholesterol/lovastin topical cream for DSAP, you're probably taking less. By my calculations, a 60 gram (or 60,000 milligram) container has 2% lovastatin, and so that's 1,200 milligrams. If hypothetically you ran out by using it twice a day for 12 weeks, that's 168 days. That's a hypothetical dosage of only 7.14 grams per application. Use it only sparingly, such as on areas that bother you most, and by my calculations this can easily reduce your intake to less than 5 grams per application. I only use about 23 grams per year, applying only to a few spots on an ongoing basis. Keep in mind that one application per day seems to work just fine.
But there's one more important question. That is whether the damage is caused only from taking in too much statin per day, or whether damage can also occur from the accumulaton of lower doses over time? If anyone knows, please let me know.
Long term prognosis?
Since DSAP is caused by a mutation of gene(s), there is no reason to believe that improvement wil be permanent.
Given the forementioned potential for liver fattening, your goal should be to use it as little as needed. Perhaps only use it on specific spots or areas that bother you.
More Details
Make sure that the compounding pharmacy sells cholesterol/lovastin (or lovastatin) in a jar -- not a pump dispenser! The pumps spit out way too much medication!
I was prescribed cholesterol/lovastin (2%/2%). One patient reports being prescribed simvastatin and cholesterol cream (2%/2%). The two medications must be mixed by a compounding pharmacy or "apothecary". Prices can vary greatly. One patient reported paying $59 for 8 ounces (226 grams). I paid $60 for 3.35 ounces (95 grams). It may be difficult to find pharmacies that sell this mixture. Click here for a list of pharmacies that sell this compounded drug combination.
You can cut off the fingers from latex gloves to use for application.
UPDATE: This study found that just taking Lovastatin 2% had the same effect as taking cholesterol 2% / lovastatin 2%.
Your Feedback Helps
Please report what happens if you try this treatment! Your feedback that I relay on this site (anonymously of course) helps all of us determine the effectiveness of various medications. Some questions that I have for others are, do you feel as though the medication helped at all after the first few weeks? Did the medication work better on your arms versus your legs? If you used this medication many months ago, is the improvement still holding up or is it starting to revert back to the previous state? Also have you had any issues with DSAP reacting (itching, redness, etc) after being administered a COVID-19 vaccine?
Harsh "brute force" medications / treatments
You want to avoid irritating DSAP spots, whether that be from picking at them, getting cut up from gardening or whatnot, or getting too much sun exposure, even while wearing the highest SPF sunscreen. Such irritation often causes DSA spots with no hyperpigmentation to become permanently reddish looking and/or to at least take a very long time for the redness to subside. That is why I caution anyone considering any harsh treatments!
After having misdiagnosed or even after having correctly diagnosed a DSAP patient, doctors will often give the patient an off-label prescription for a topical medication called Efudex (AKA Fluorouracil, Fluorouplex, Carac), which only makes DSAP look horribly red and irritated for many weeks during treatment and then for a few months afterward while really doing nothing to improve the skin condition. Why would it help? DSAP is, of course, rooted in gene expression. This is not like trying to treat ringworm or a common wart. After reviewing many emails and guestbook posts I have come to my own conclusion that Efudex is an aggravating waste of time when it comes to 'treating' DSAP.
It appears as though other harsh treatments such as Tazorac, Retin-A, and Aldara are also an aggravating waste of time. I have not received one single report of these meds clearing up DSAP.
Based on reports, I would also avoid Levulan light therapy or "Blue Light" therapy. I've had four reports on this treatment and they were all negative.
"Chemical" peel
Here's a study out of Germany that claims good results on 5 patients using glycolic acid 50% and salicylic acid 25%, treating 3 times, 6 weeks apart. The study claims better results than other 'brute force" treatments. No information was provided regarding hyperpigmentation during and after treatment, and no information was provided as far as long-term results.
I am always skeptical of these 'brute force' type treatments. Why would this treatment yield any better results than freezing, laser treatment, etc. And why would anyone expect improvement to hold up long-term since DSAP is rooted in gene expression?
As with all 'brute force' type treatments, I recommend doing only a test spot to start. Also, one has to wonder if first applying cholesterol/lovastatin twice a day for 4 weeks or so to your test spot would help prepare the test spot for better results, or allow you to reduce the number of glycolic acid / salicylic acid treatments, perhaps from three to two. Note that glycolic acid 50% and salicylic acid 25% are available over-the-counter. I don't know if these meds are applied separately or as one mixture.
"Successful use" of Grenz Rays reported
Click here for details. This report indicates 7 of 8 patients had success with grenz rays treatment. Patients experience temporary side effects, apparently red and very itchy spots for a few weeks, before clearing up. One patient reports that the treatment itself doesn’t hurt at all. This patient also reports that 3 years later the DSAP spots are still gone.
While Grenz rays are reported as safe, they are nonetheless x-rays and thus should be treated with the same amount of caution as with other ionizing radiation. There is continuing concern about the potential cancer risk in any patient treated with ionizing radiation. Some studies (Dabski and Stoll, as well as R. Mortensen and Kjeldsen) have reported incidences of cancer following grenz ray treatments. However, one study from a Swedish cancer registry concluded that "if there was any risk of skin malignancies, it would be very small."
As always, I have to question how does this treatment hold up a month or more after treatment? And, I am just skeptical of any and all harsh treatments, especially if improvement might not hold up.
Report of DSAP cleared from Ozone Therapy
YouTube video , Doctor's website . Apparently this patient developed DSAP in short order after brain surgery. Unless he also had radiation therapy or he was relaxing in the sun a lot, this doesn't make sense. DSAP develops from years of sun exposure, although the redness of DSAP eventually presents itself relatively suddenly. So I have to question if he really had DSAP (it's often misdiagnosed) or if he had some strange variant of DSAP. Could this treatment be confused for "spontaneous resolution" as discussed at the bottom of this page (in the blue box)? Ozone therapy carries risk. Scroll down to "Is it safe?" I am always skeptical of single reports of DSAP clearing, as well as lone doctors using a treatment. Some of the questions I would ask would be how many DSAP patients have experienced skin clearing from using this treatment? And for how many people did it not work? And most importantly, there is no information about how long this treatment lasts for. For me personally, the safety of this treatment strikes me as being too sketchy, especially if I don't even know if improvement will be permanent or not. Unless the gene mutation is addressed, it just doesn't make sense to me that any "successful" treatment would hold up over time.
2 reports of full resolution of DSAP and 2 reports of the treatment doing nothing
Here is a report about an 80-year old woman being successfully treated with a combination of topical calcipotriol (a vitamin D3 analog) and betamethasone gel (a corticosteroid). Significant improvement was seen after only 3 weeks, and "almost full resolution" in the second month of treatment.
Why would two meds that are ineffective by themselves somehow perform successfully when used together? If anyone has tried or prescribed this combination of meds please report the results back to me. I am always skeptical of these lone reports, however I have since received a personal email from someone who is also reporting success...
YET ANOTHER SUCCESS STORY: 1/15/2018 - I received a "success story" email from someone with DSAP who reports using the above combination of Betamethasone dipropionate cream .05% (manufactured by Fougera) and Calcipotriene Cream .005% (manufacturer Sandoz) for 20 days. For the first 10 days nothing happened, but then the area treated became very red, much like what you would see with an actinic keratosis patient using Edudex. This person reports that it became so inflamed that they were worried that there would be some sort of permanent damage / scarring left behind. However after about a week or two the redness and scaling went away as did the DSAP. After a year there has been no return of DSAP.
 BAD NEWS: 4/22/2018 - Unfortunately I received another report from someone who tried the above regimine for 20 days. About a month after ending treatment they were back to square one. The treatment did not help at all.
BAD NEWS: 4/22/2018 - Unfortunately I received another report from someone who tried the above regimine for 20 days. About a month after ending treatment they were back to square one. The treatment did not help at all.
 MORE BAD NEWS: 8/6/2018 - Yet another report of this treatment having "absolutely no effect whatsoever". This person used Betamethasone Dipropionate and Calcipotriene 0.005% cream.
MORE BAD NEWS: 8/6/2018 - Yet another report of this treatment having "absolutely no effect whatsoever". This person used Betamethasone Dipropionate and Calcipotriene 0.005% cream.
Please report back your results whether positive or negative if you try this combination treatment. I am told that you may be able to try this treatment at no cost. Have your MD call PruGen Pharamaceutical ($0 Co-Pay) through a mail order program called GenRx2U: www.GenRx2u.com or 1-844-436-7928. I just don't believe that this treatment works and I don't like any treatment that causes inflammation/ redness.
Important discovery made at Anhui Medical University in China
NEWS STORY - Sept 16, 2012 - A team of researchers at Anhui Medical University in China and BGI has found strong evidence that there is a link between mutations of the mevalonate kinase gene (MVK) and DSAP. It is a major step toward discovering the genetic mechanism that causes DSAP, and sheds light on its further molecular diagnosis and treatment. According to Tao Jiang "Our study provides new insights into the pathogenesis of DSAP, and the identified MVK mutations offer the best candidate targets for gene diagnosis and clinical treatment of the disease". According to Xuejun Zhang, President of Anhui Medical University, this study "provides scientific basis for revealing DSAP pathogenesis, genetic counseling, risk prediction, prenatal diagnosis, new drug development, clinical diagnosis and treatment." Let's hope that this leads to a gene therapy sooner than later.
Report of DSAP 'effectively treated' with ingenol mebutate gel
Here's a report of DSAP being "treated effectively" with ingenol mebutate gel 0.05% (AKA Picato Gel). According to the article, this med causes an inflammatory response (redness and scaling) but with no blistering, swelling or ulceration. Treatment only requires 2 days of application. Ingenol mebutate is derived from the sap of milk weed. By day 60 there was improvement seen with this patient. Ask your doctor about trying a test spot or two. Unfortunately I am discovering that this medication is $750 per tube! However sometimes you can find medications at drastically cheaper prices in places like Europe and Mexico.
UPDATE: One DSAP patient has reported trying Picato Gel twice to no avail.
If you experiment with this med then please report back what happens. Your feedback helps!
Diclofenac sodium topical gel 1%
For what it's worth, I received two emails from patients who were prescribed the topical anti-inflammatory drug Diclofenac. One was very pleased with results using 3% Diclofenac, but when they ran out of medication after just a few months their condition "got bad again". More recently someone emailed me saying that Solaraze did nothing. But remember that doctors are famous for prescribing meds like Efudex and other waste-of-time and money drugs that do nothing to clear up DSAP.
So I tried testing out using 5% Diclofenac on some test spots. After 11 months it did nothing. For the last 8 months I increased test spot applications to twice per day. This leads me to believe that any reports of Diclofenac actually "working" actually may be a case of it working on spots of actinic keratosis or some other condition -- not dsap. Sometimes doctors confuse the two, or patients could have a combination of the two conditions. Also Diclofenac seems to somewhat restrict blood flow to the application area, much the way Desowen cream temporarily makes skin look clear. After all Dicofenac is an anti-inflammatory. I believe this may explain the positive reports about Diclofenac that I've received.
I am trying to gather more reports on this drug from others who may email me. The other email I received was from someone who says that they visited a dermatologist who looked at their DSAP and declared "I have a cure for that". This sounds absurd to me. There is no cure. If there was then this would be front page news in the dermatology community. I believe this is just another case of a doctor who either doesn't know what they are talking about or is trying to fraudulently drum up repeat patient visits, which increase the doctor's income. This doctor has apparently prescribed Voltaren Gel to be used once in the evening for 6 months to a year. That's a long time but there is not supposed to be any harsh reaction, like you would experience with other meds like Efudex. This doctor believes that DSAP is somehow rooted in inflammation. This further indicated to me that this doctor doesn't know what they are talking about. If anyone else has any stories to report on Disclofenac for DSAP then PLEASE email me. Again I am in the very early stages of gathering reports about this med. I am told that Diclofenac is $150 per tube with insurance --or $800 without! However another patient living outside the country reports that Voltaren costs only 10 USD. Upon further research I've found Mexican online pharmacies that charge only $25.75 and probably don't require a prescription. Another from Bulgaria sells Diclac 5% on Ebay for about $18 including shipping. Speak to your doctor about using Voltaren.
Welcome side effect from chemotherapy
I have received two reports from DSAP patients who were delighted to see their DSAP spots "shed off" as a side effect from being on chemotherapy, but both reported that DSAP simply grew back a year or two later.
Dovonex / Tacalcitol / Calcipotriol
I've found two reports of DSAP patient's skin clearing from using Tacalcitol and from Calcipotriol. My doctor says that this drug has worked for one patient of his, but not others. My impression is that this drug works for very few patients. In all of my years of running this site and receiving emails from patients, I haven't ever heard from one single patient who had success from using topical D3 analogs like Tacalcitol, which is usually prescribed for psoriasis. In the USA, Calcipotriol is sold under a different name called Dovonex. As far as I can tell, it can't hurt to try Dovonex or Calcipotriol because (unlike drugs like Efudex) there is no harsh reaction from using this topical cream. I tried it. It did absolutely nothing. I've never heard from anyone else who said that it caused any harsh reaction.
Avoiding both the sun and harsh medical treatments may be your best course of action
One thing that really does help for DSAP improvement over time is simply using the strongest sunscreens and avoiding direct sunlight as best you can. I promise you will see improvement! This is especially true when you consider that when patients are first diagnosed with this condition, cosmetically it is usually at its very worst. Often this is because patients had been hanging out in the sun with little regard for the need for strong sunscreen.
Does this mean that you can't walk in and out of parking lots during the summer while wearing SPF-100? No. Instead I would avoid something like a leisurely walk on a beach boardwalk during the summer. Even while wearing SPF-100 sunscreen, if you spend enough time in the sun, DSAP spots will start to show some redness.
Also avoid all of the harsh treatments described on this site. They will only cause additional cosmetic setback. I believe that some of the redness of DSAP is maybe a bit like the knees you scarred as a kid. It can take a long time for that redness to improve once you commit to giving your skin a chance to recover. And when combined with some creative use of sunless tanners you can actually find yourself looking pretty normal again.
Lack of sun exposure has been linked to high blood pressure
As a note of warning, you might want to think about getting at least some sun exposure for the vitamin D benefits as well as other benefits. Sunlight alters levels of the messenger molecule nitric oxide in the skin and blood, which in turn reduces blood pressure.
All of this doesn't mean that you should be getting sun on areas that are affected by DSAP, such as arms and legs. Your back is a nice large area to soak up lots of ultra-violet rays. You don't want to burn either. Visit this page for helpful information on sun exposure.
Also take vitamin D and Vitamin K supplements.
Current "treatment" for DSAP is only said to be suppressive or palliative (to try to make appear less offensive) rather than curative. Most patients (especially myself and those with light complexions) will argue that these harsh "palliative" treatments (like Efudex, lasers, freezing, and others) are a waste of effort and will worsen your appearance short term and may even worsen your long term appearance. I have however read and received reports of people's varying degrees of improvement from deep freezing and from using laser treatment, but for every positive report I get a negative report from patients who tried freezing but wound up looking worse or no better long term. Accordingly save yourself the aggravation; If you decide to venture down the freezing or laser treatment route I suggest trying only a test spot or two to start. Read some of the guestbook posts in this site BEFORE trying any treatment. Email as many people as you can with questions. Again, people with very fair skin might be best suited to just avoid freezing or laser treatment.
My gut feeling is that the only real DSAP treatment that will ever really work will emerge from an off label use of medication(s) intended for psoriasis and/or actinic keratosis, or emerge someday from proteonics (protein expression) or better yet from stem cell therapy. Hopefully more studies like the one in China will continue. One of the first hurdles in getting research under way is finding patients to donate DNA samples. Fortunately as a result of maintaining this page for over ten years I already have contact info for many DSAP patients. I would expect that a good number of these people would be more than happy to help in research studies if one ever materializes.
DSAP is considered a rare disorder so most dermatologists have little (if any) experience with "treatments". Therefore it would be wise to do your OWN foot work and second guess your doctor's "treatment" advice, especially if they want to put you on a harsh treatment like Efudex, or chemical peel or extensive freezing treatment without trying test spots first and waiting several months. When first diagnosed, DSAP patients are often desperate to "try anything", and doctors feel compelled to at least "try something", however the best path may just be to simply make an effort to avoid the sun, wear strong sunscreen and take no medications at all, or maybe try "test spots" with various medications and/or freezing. Ask your doctor how many patients he/she has worked with. Just how knowledgeable is he/she? Does your doctor even know what DSAP is? It is YOUR OWN responsibility to find a knowledgeable doctor! Based on my experience there are very few who know their field inside and out. I believe that you might be best off finding an older (experienced) doctor who has practiced a long time and works out of an office with perhaps other dermatologists from whom they can get 2nd opinions. DSAP mainly affects people of European decent (white people) so perhaps you might get better diagnosis from a Caucasian doctor. There seems to be too little knowledge on the disorder. Much of the knowledge that IS out there is clouded and confused. But after reading this page YOU might become more knowledgeable on DSAP than the vast majority of dermatologists! I have sorted through the mess (by scouring the net, talking to some doctors and many patients) and finally created this page to share my experience, and for all of us to gather info from around the world about DSAP. Bookmark www.dsap.net and periodically check back for the latest DSAP news.
Some facts about DSAP:
Analysis of DSAP shows altered DNA ploidy, chromosomal instability, and abnormal over-expression of tumor suppressor p53 protein.
DSAP is characterized by annular (round-ish), dry patches (or lesions) that eventually become pigmented (red, brown) with continued sun exposure, and (from my experience) from scratching /picking, and time. In a perfect world doctors would be able to identify DSAP years in advance when only a few faint round outlines of DSAP are becoming visible, with no discoloration (or sometimes with even HYPO-pigmentation). Areas affected are usually sun exposed areas of the arms and /or legs. I've read about other areas of the body being affected such as the back and belly. It affects the LEGS of women more than men (I have to theorize that this may be from wearing dresses rather than from genetic reasons). In men it is said to affect the arms more (than legs). In about 15% of patients the cheeks of the face are affected, otherwise (oddly enough) the face is usually spared. If a male patient has keratotic spots on their arms and / or legs but NOT on their face, a savvy doctor will pick up on this (as more of an indicator of DSAP than Actinic Keratosis). But don't rule out that AK (or DSAP) may be less prevalent on a female patient's FACE due to habitually wearing makeup (which can contain or simply act as a sunscreen). Nearly 1/3 of patients experience minor itching. DSAP is said to affect both sexes evenly. The average age at which patients start to see DSAP become prominent is about 40.
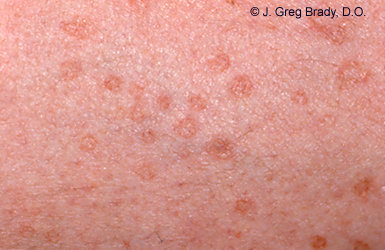
RIGHT: These are smaller DSAP spots. Perhaps a few years earlier these spots appeared as nothing more than very slight raised borders (with NO discoloration) viewed only up close by a discriminating eye against a backdrop of light, and dry skin. The difficulty in getting early detection is that DSAP doesn't appear with hyper-pigmentation (redness) until years after the accumulated sun exposure. People who have been so lucky as to get diagnosed very early on (before there is hyper pigmentation) really need to wise up to the fact that they need to make lifestyle changes and stay out of the sun starting NOW! There is a phenomenon about DSAP that I have noticed (and so have other patients who have emailed me) and that is that the redness of DSAP spots always seems to become prominent rather suddenly. Perhaps all in one summer it suddenly becomes a very noticeable cosmetic issue. Larger DSAP spots typically aren't as perfectly round as depicted in this photo shows.
In most cases DSAP is inherited, but sometimes people develop DSAP (or at least have very high susceptibility to develop DSAP) when their immune systems are not working well. Radiation therapy can severely exacerbate DSAP! You don't even want to see the horrific photos of DSAP lesions that develop after going through radiation cancer therapy.
A disservice paid to patients by dermatologists is the failure to inform DSAP patients about hereditary factors. It is vital that family members be informed if a parent (or sibling) has been diagnosed as having DSAP spots! In the late 1960's it was concluded by a researcher that DSAP acts autosomal hereditary. From my understanding of heredity, each offspring has a 50% chance of inheriting the DSAP gene if one parent has the faulty "DSAP gene". If both parents have the DSAP gene then I believe there is either a 50% or 75% chance of gene transmission. With these odds I'd say family members might like to know the risks! Keep in mind that a certain level of sun exposure is required before the lesions appear on the skin. For example: one may have the DSAP gene BUT live in long sleeve climate, or habitually avoid the sun, or habitually wear sunscreen thus NEVER developing DSAP spots or significant DSAP spots. DSAP is brought on by sun exposure BUT other factors may be involved. DSAP lesions have "thread-like" outer boarders, making them perhaps look sort of like craters on the moon when viewed at an angle against a backdrop of light. (Note: These "raised borders" are in actuality much smaller than sewing thread. Also the "thread-like" borders are much less noticeable when skin is wet from vitamin E, sun screen, etc. Skin should be DRY and oil free to really see the characteristic defined borders.) DSAP spots usually encircle pore(s) that are sort of "hardened", clogged, not functional, and stick up slightly. DSAP has been labeled as "pre-cancerous" but development of true skin cancer in DSAP is "uncommon" and in fact one study seemed to suggest that the only DSAP patients who developed cancer were those who very irresponsibly continued to be exposed to the sun. For most people DSAP is a cosmetic problem and a lifestyle changing problem but NOT a cancer concern. Note that I have received emails from people who have had DSAP for 40 years and been cancer free. As of 2023, I have had DSAP spots for about 32 years and no spots have become cancerous. DSAP is unlike actinic keratosis, which can develop into cancer within 6 months. I have heard talk of DSAP "remission" but it appears that those who develop DSAP slowly over the years do NOT experience remission.
I e-mailed a doctor who authored a web page that spoke of DSAP "spontaneous resolution":
MY QUESTION: Your article on DSAP reads "Protection from ultraviolet radiation may lead to spontaneous resolution." and "Lesions may resolve with discontinuation of ultraviolet exposure." I'm wondering just how rare or common this occurrence can be. Have DSAP patients seen their skin clear up?
RESPONSE: Yes, DSAP patients have seen their skin clear up after exposure to ultraviolet radiation is discontinued. I cannot give you a percentage for resolution. The reports of this occurrence generally have a clear causal relation, eg. fair skinned European who goes to the beach for 6 weeks, develops DSAP, which then resolves after protection from further ultraviolet exposure.
MY QUESTION: 6 weeks? OK. What about patients who develop DSAP slowly over the years. Is reversal seen in these instances?
RESPONSE: Improvement is seen, but not complete resolution. Reduced risk of malignant
degeneration is the major reason to protect from ultraviolet radiation.
CLICK HERE to continue reading about DSAP
BELOW: Creative masking technique + sunless tanner = A nifty cosmetic solution
HOME | CONTINUED | RESEARCH | COSMETIC SOLUTIONS | OFF-LABEL DRUG USE | PRODUCTS | LASERS & FREEZING | GUESTBOOK | CONTACT
Since 12/25/2001